Main menu
Common skin conditions
NEWS
Join DermNet PRO
Read more
Quick links
Subacute cutaneous lupus erythematosus — extra information
Autoimmune/autoinflammatory Rashes
Subacute cutaneous lupus erythematosus
Authors: Dr Helen Gordon, Dermatology Registrar, New Zealand. Adjunct A/Prof. Amanda Oakley, Dermatologist, New Zealand. July 2019. Minor update Dr Ian Coulson, Dermatologist, June 2023.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
What is subacute cutaneous lupus erythematosus?
Subacute cutaneous lupus erythematosus (SCLE) is a subtype of cutaneous lupus erythematosus. It presents as a widespread non-scarring photosensitive rash.
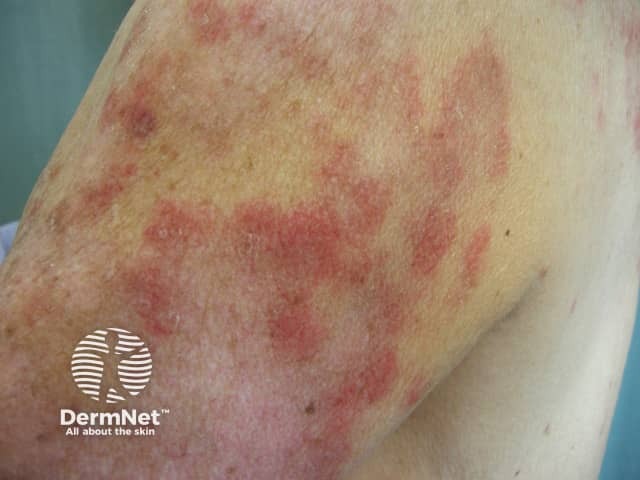
Drug-induced subacute lupus erythematosus
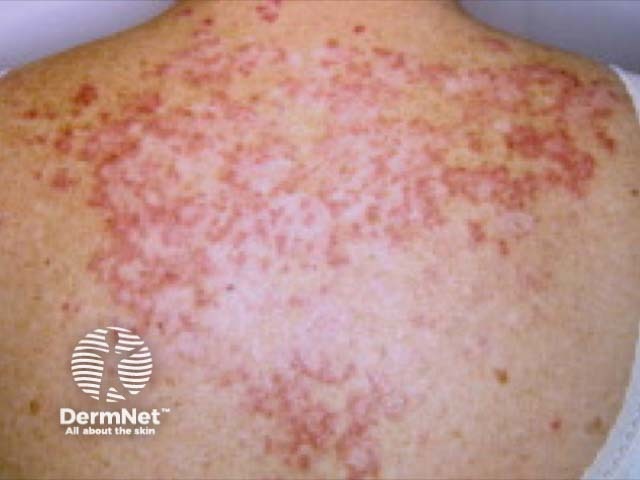
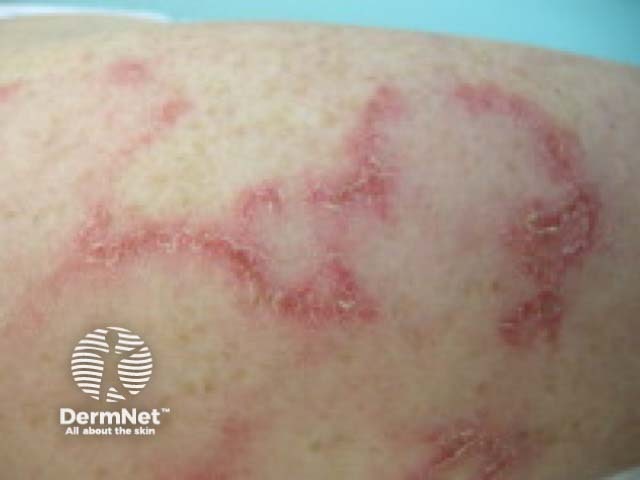
See more images of cutaneous lupus erythematosus.
Who gets subacute cutaneous lupus erythematosus?
SCLE affects about 10% of all patients with lupus.
- Patients can be of any age, sex, or ethnicity. However, SCLE is most often diagnosed in middle-aged women.
- In North America, SCLE is more common in Caucasians than other ethnicities.
- It can be associated with other diseases, including Sjögren syndrome, rheumatoid arthritis, and Crohn disease.
What causes subacute cutaneous lupus erythematosus?
SCLE is due to genetic and environmental factors.
Genetic factors
SCLE is associated with the human leukocyte antigen (HLA)-A1-B8-DR3-DQ2-DRw52-C4null ancestral haplotypes. Other genetic associations include:
- Deficiencies in complement proteins component (C)2 and C4
- Polymorphisms in the tumour necrosis factor (TNF)-alpha promoter gene.
Environmental factors
Immune tolerance is lost or autoimmunity develops through exposure to environmental triggers such as exposure to ultraviolet radiation (UVR) or photosensitising drugs.
Exposure to UVR results in increased expression of the Ro/SSA antigen on the surface of keratinocytes, binding the anti-Ro/SSA antibody and leading to the disease.
It is estimated 20-40% of cases of SCLE are drug-induced. The incubation time widely varies from a few days (such as in the case of the chemotherapy agents capecitabine and paclitaxel) to years before the onset of the rash (eg, a case was reported to arise 5 years after starting a thiazide diuretic).
The drugs most commonly associated with SCLE are:
- Thiazide diuretics
- Terbinafine
- Calcium channel blockers.
Other drugs that may cause SCLE include:
- Tamoxifen
- Lansoprazole
- Statins
- Angiotensin-converting enzyme (ACE) inhibitors
- TNF-alpha inhibitors
- Leflunomide
- Carbamazepine
- Docetaxel
- Paclitaxel
- Capecitabine
- Inhaled tiotropium
- Naproxen.
Other associations
Malignancy: there are increasing reports of SCLE being temporally associated with underlying cancers, including carcinoma of the lung, oesophagus, prostate, cholangiocarcinoma, and B-cell lymphoma.
What are the clinical features of subacute cutaneous lupus erythematosus?
SCLE most often presents as a non-scarring papulosquamous eruption.
- Typically, there are annular plaques with raised erythematous borders and central clearing.
- The plaques coalesce to form polycyclic patterns.
- They may or may not have an overlying scale.
- Sometimes, there are peripheral vesicles, crusting, and bullae.
- The rash is typically symmetrically distributed on the sun-exposed sites of the neck, the upper trunk, and the outer arms.
- The face is usually unaffected.
- Lesions resolve with post-inflammatory hypopigmentation; normal pigmentation recovers over time.
Other lupus-associated findings in patients with SCLE include:
- Diffuse non-scarring alopecia (50%)
- Mouth ulcers
- Livedo reticularis
- Periungual telangiectasia.
Drug-induced lupus can be indistinguishable from the non-drug-induced form of SCLE. Specific features of drug-induced SCLE include:
- Usually presenting in older patients
- Association with a likely drug
- Malar rash
- Involvement of the legs
- Bullous, targetoid, or vasculitic variants.
What are the complications of subacute cutaneous lupus erythematosus?
Around 50% of patients with SCLE meet the American College of Rheumatology criteria for the diagnosis of systemic lupus erythematosus (SLE).
A pregnant woman who is Ro/SSA antibody-positive has a risk of delivering an infant suffering from neonatal lupus erythematosus (8–10%) and congenital heart block (1–2%).
How is subacute cutaneous lupus erythematosus diagnosed?
SCLE can be diagnosed clinically, supported by the results of blood tests and a skin biopsy.
- Around 60% of patients with SCLE are antinuclear antibody (ANA) positive
- More than 80% are Ro/SSA antibody positive
- La/SSB, dsDNA, anti-histone, and Sm antibodies are less common.
The histology on biopsy can resemble other forms of cutaneous lupus.
- There is a lymphocytic interface dermatitis with basal layer degeneration.
- Epidermal atrophy and apoptotic keratinocytes are more prominent than in discoid lupus erythematosus (DLE).
- Perivascular and periadnexal lymphocytic infiltrate, follicular plugging, basement membrane thickening, and dermal mucin are less prominent than in DLE.
- Direct immunofluorescence reveals a granular deposition of immunoglobulin (Ig)G, IgM, and C3 along the dermal–epidermal junction in approximately two-thirds of patients with SCLE (the lupus band test).
Drug-induced SCLE and non-drug-induced SCLE cannot be distinguished on histology.
What is the differential diagnosis for subacute cutaneous lupus erythematosus?
The differential diagnosis for SCLE includes other types of cutaneous lupus, especially:
Other skin conditions that may be considered include:
- Dermatomyositis
- Erythema annulare centrifugum
- Other forms of annular erythema
- Granuloma annulare
- Lichen planus
- Psoriasis
- Nummular eczema
- Tinea corporis.
What is the treatment for subacute cutaneous lupus erythematosus?
General measures
Sun protection is crucial.
- Seek shade when outdoors.
- Wear covering, sun-protective clothing.
- Apply a broad-spectrum sunscreen to uncovered areas.
Topical therapy
Topical therapy may include:
Oral therapy
The main treatment for SCLE is an antimalarial drug, particularly hydroxychloroquine. Antimalarial drugs are less effective in smokers.
In approximately 25% of cases, another agent is required, such as:
- An oral corticosteroid
- An oral retinoid (acitretin or isotretinoin)
- Dapsone
- Methotrexate
- Mycophenolate
- Etanercept
- Thalidomide.
What is the outcome for subacute cutaneous lupus erythematosus?
SCLE generally responds well to treatment, although it may flare up again each summer.
Approximately 10–15% of patients with SCLE develop SLE, including renal and neurological involvement.
Drug-induced SCLE can be slow to resolve on stopping the causative drug (one study found resolution took a mean of 7 weeks).
References
- Lupus erythematosus. In: Griffiths CE, Barker J, Bleiker T, Chalmers R, Creamer D (eds). Rook's textbook of dermatology, 9th edn. Chichester: Wiley‐Blackwell, 2016.
- Sontheimer RD. Subacute cutaneous lupus erythematosus: 25-year evolution of a prototypic subset (subphenotype) of lupus erythematosus defined by characteristic cutaneous, pathological, immunological, and genetic findings. Autoimmun Rev 2005; 4: 253–63. DOI: 10.1016/j.autrev.2004.10.003. PubMed
- Hillesheim PB, Bahrami S, Jeffy BG, Callen JP. Tissue eosinophilia: not an indicator of drug-induced subacute cutaneous lupus erythematosus. Arch Dermatol 2012; 148: 190–3. DOI: 10.1001/archdermatol.2011.290. PubMed
- Marzano AV, Lazzari R, Polloni I, Crosti C, Fabbri P, Cugno M. Drug-induced subacute cutaneous lupus erythematosus: evidence for differences from its idiopathic counterpart. Br J Dermatol 2011; 165: 335–41. DOI: 10.1111/j.1365-2133.2011.10397.x. PubMed
- Lowe G, Henderson CL, Grau RH, Hansen CB, Sontheimer RD. A systematic review of drug‐induced subacute cutaneous lupus erythematosus. Br J Dermatol 2011; 164: 465–72. DOI: 10.1111/j.1365-2133.2010.10110.x. PubMed
- Tiao J, Feng R, Carr K, Okawa J, Werth VP. Using the American College of Rheumatology (ACR) and Systemic Lupus International Collaborating Clinics (SLICC) criteria to determine the diagnosis of systemic lupus erythematosus (SLE) in patients with subacute cutaneous lupus erythematosus (SCLE). J Am Acad Dermatol 2016; 74: 862–9. DOI: 10.1016/j.jaad.2015.12.029. PubMed
- Merola JF. Overview of cutaneous lupus erythematosus. UpToDate. Available at: www.uptodate.com/contents/overview-of-cutaneous-lupus-erythematosus (accessed 9 June 2019).
- Xie F, Frewen J, Divekar P. Three cases of subacute cutaneous lupus erythematosus associated with malignancy: a late paraneoplastic phenomenon. Clin Exp Dermatol. 2020;45(5):607-608. doi:10.1111/ced.14176 Journal
On DermNet
- Cutaneous lupus erythematosus
- Cutaneous lupus erythematosus images
- Psychological impact of cutaneous lupus erythematosus
- Drug-induced lupus erythematosus
- Discoid lupus erythematosus
- Discoid lupus erythematosus pathology
- Systemic lupus erythematosus
- Systemic lupus erythematosus images
- Chilblain lupus erythematosus
Other websites
